July 4, 2025, 8:09 pm | Read time: 6 minutes
People love to chat about all sorts of minor ailments. But athlete’s foot? No one talks about it. Yet, tips would likely be very welcome—such as how to prevent infection, recognize symptoms, and treat athlete’s foot.
Even though the thought is unpleasant, fungi are everywhere on the skin. They only become a problem when they enter the skin through small cracks or injuries and cause inflammation. This can lead to athlete’s foot, which is much more than a cosmetic issue. If untreated, it can spread along the foot to the heel and up the thighs to the buttocks. If it affects the nails, they become rough, brittle, and crumbly. Therefore, early treatment is crucial.
Follow the FITBOOK channel on WhatsApp now!
Overview
Recognizing and Treating Athlete’s Foot
Typical Symptoms Include:
- Persistent itching, especially between the toes, that does not subside despite care.
- Soft, moist skin areas between the toes, often with whitish deposits and an unpleasant odor.
- Redness, skin scaling, or blistering between the toes, sometimes accompanied by pustules.
- Dry, scaly skin areas on the sole of the foot, often whitish or slightly reddened.
- Thickened calluses, scaling, or fine skin cracks at the edges of the feet, sometimes with a feeling of tightness.
For treatment, healthy adults can first try to tackle the fungus on their own: appropriate creams, gels, and sprays for fungal infections are available over the counter at pharmacies. They are applied once or twice daily over a large area around the affected areas.
What patients should never do: simply stop the therapy. Even if the symptoms subside quickly, the therapy should continue for at least two weeks.1
Also interesting: The different forms of skin fungus and their symptoms
These Variants Exist
Athlete’s foot is differentiated based on which skin areas are affected and the pattern of symptoms.2
Athlete’s Foot Between the Toes (Interdigital Type)
This is by far the most common variant. It mainly occurs in the spaces between the fourth and fifth toes, as it is most often moist and poorly ventilated there. The first signs are usually softened skin areas. As it progresses, redness, scaling, and painful cracks may develop. An unpleasant odor often accompanies it.
Scaling Athlete’s Foot (Squamous-Hyperkeratotic Type/Moccasin Type)
This form primarily affects the soles of the feet, often the edges and heels as well. It is characterized by dry, scaly skin with fine cracks. The inflammatory reaction is usually only mildly pronounced. In advanced stages, the scaling can intensify, especially on the heels, leading to deep and painful fissures. The pattern of infection often resembles a moccasin, hence the term “moccasin form.”2
Athlete’s Foot with Blisters (Vesicular-Dyshidrotic Type)
This variant is characterized by small, itchy blisters that appear mainly on the soles and edges of the feet. The blisters are often filled with fluid but do not burst on their own due to the strong skin scaling. Instead, they dry out and form crusts. The associated feelings of tightness, itching, and signs of inflammation are often particularly pronounced.
Causes and Risk Factors
Whether at the swimming pool, sauna, or hotel room–walking barefoot in these places exposes your feet to increased risk. Fungal spores thrive on warm, moist floors and need only a minimal entry point: a softened skin area, a small injury, or cracks between the toes. Once they enter the skin this way, athlete’s foot can develop.
The most common pathogens are so-called dermatophytes, which are filamentous fungi that prefer to settle in the horny substance of the skin. However, yeast or mold fungi can also cause an infection.3 Particularly favorable conditions arise when feet are enclosed in non-breathable footwear for extended periods. Wearing synthetic socks or excessive sweating creates a consistently warm, moist environment, ideal for the spread of pathogens.
Other risk factors include a weakened immune system, such as from pre-existing conditions, certain medications, or high stress. Chronic diseases like diabetes mellitus increase the risk because they impair blood circulation in the feet and make the skin more susceptible to damage. Circulatory disorders in old age or limited foot care also promote the development of athlete’s foot.
Hygiene plays a crucial role: failing to thoroughly dry your feet after washing, especially between the toes, or not wearing shower shoes in communal facilities can make it easier to contract the pathogens.
Also interesting: How often can you shower without harming your skin?
When to Seek Medical Advice
Athlete’s foot can often be effectively treated with over-the-counter products from the pharmacy. However, there are situations where medical advice is essential. This is especially true if symptoms do not improve within two to three weeks of treatment or worsen. Medical evaluation is also necessary for recurring infections or severe symptoms like painful cracks, oozing skin areas, or blistering.
Special caution is advised for people with a weakened immune system. This includes those with diabetes mellitus, circulatory disorders, or those taking certain medications. Older adults or individuals with limited mobility who cannot adequately inspect their feet should seek medical help at the first signs.
Finally, seeking medical advice can also be beneficial for diagnostic reasons: not every redness or scaling on the foot is automatically a fungal infection. Eczema, psoriasis, or bacterial skin diseases can cause similar symptoms. An accurate diagnosis allows for targeted therapy and prevents unnecessary treatment attempts with unsuitable remedies.
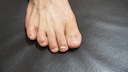
Early Signs to Recognize Nail Fungus

Dry, Flaky Nipples in Women – Causes and Treatment
Tips for Prevention
Once the athlete’s foot infection has healed, precautions should be taken to avoid catching another fungus. Caution is advised in places where many people walk barefoot, such as public baths, wellness facilities, and saunas, as well as hotel rooms. It’s best to always wear shower shoes. It’s also advisable to keep feet and the spaces between toes dry.
Preventing athlete’s foot also involves wearing well-fitting and comfortable shoes made of breathable material to quickly wick away foot moisture. Alternating showers and baths stimulate blood circulation in the feet and keep them warm in winter, preventing cracks in the skin that can lead to athlete’s foot.
What to Do if Athlete’s Foot Keeps Coming Back?
If athlete’s foot recurs after an infection subsides, it may be helpful to apply a broad-spectrum antifungal cream or spray to the feet once or twice a week as a preventive measure. These medications work against multiple pathogens, typically using active ingredients from the pyridone or azole groups.
Living a healthy lifestyle with a vitamin-rich diet, exercise, and adequate sleep also strengthens the immune system, contributing to protection against athlete’s foot.
*With material from dpa

